Wounds, Drains & Dressings: The Unfiltered Truth
- Vanessa Chambers

- Feb 19
- 3 min read
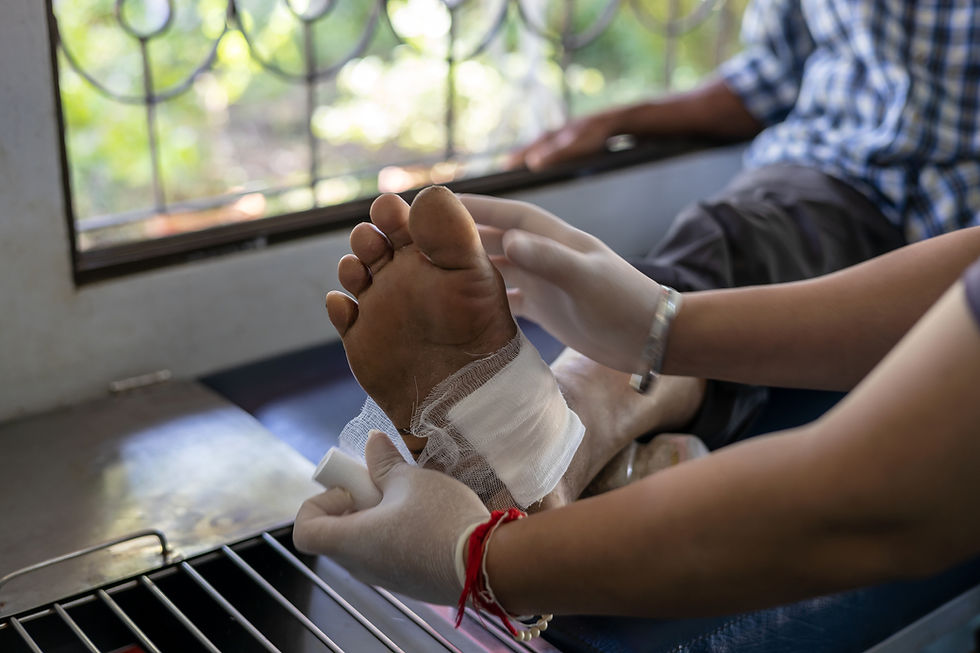
Surgery does not end in the operating room. Recovery begins the moment the incision is closed.
For many post-operative patients, especially orthopedic, abdominal, and reconstructive procedures, the greatest anxiety happens at home. Not because of pain alone, but because of the wound itself.
1. The Surgical Wound: What Is Normal?

A surgical incision is a controlled injury created under sterile conditions. Healing occurs in predictable phases:
Hemostasis (First 24 Hours)• Mild oozing or spotting on the dressing• Swelling around the incision• Bruising that may extend beyond the surgical site
Inflammatory Phase (Days 1–5)• Redness at the edges (1–2 cm is typically normal)• Warmth around the site• Mild firmness or tenderness• Clear, pink, or light yellow drainage
Proliferative Phase (Days 4–21)• Edges begin sealing• Scab formation or surgical glue sloughing• Decreasing redness and swelling
Maturation Phase (Weeks to Months)• Scar remodeling• Color changes (red → pink → pale)• Flattening of raised areas
Not every change is infection.Understanding the difference is critical.
2. When Red Flags Matter

Contact your surgeon or nurse immediately if you observe:
• Expanding redness (>2–3 cm from incision)• Thick, green, or foul-smelling drainage• Sudden increase in swelling• Fever over 100.4°F• Wound edges separating• Increasing pain instead of gradual improvement
Early intervention prevents complications such as cellulitis, dehiscence, or abscess formation.
3. Drains: Why They Exist & What They Mean

Post-operative drains (JP drains, Hemovac, etc.) are placed to:
• Prevent fluid accumulation• Reduce hematoma formation• Minimize infection risk• Protect surgical repairs
Normal drain output: • Initially dark red → light red → pink → straw-colored• Gradual decrease in volume over days
Concerning drain output: • Sudden spike in volume• Bright red blood after several days• Milky or cloudy fluid• Strong odor
Drain care is not cosmetic. It is clinical surveillance.
Improper emptying, failure to measure output, or poor anchoring can compromise recovery.
4. Dressings: Clean Is Not Always Sterile

Many patients are surprised to learn that:
• Not all wounds require daily dressing changes
• Over-cleaning can delay healing
• Hydrogen peroxide is rarely appropriate
• Occlusive dressings can promote faster epithelialization
Your dressing type may include:
• Steri-strips
• Surgical glue
• Silver-impregnated dressings
• Foam dressings
• Negative pressure wound therapy
Each serves a specific purpose based on wound depth, tension, and risk profile.
5. The Psychological Impact of Surgical Wounds
Scars can carry emotional weight.
Post-operative patients may experience:
• Anxiety about appearance
• Fear of infection
• Hesitation to shower or mobilize
• Hypervigilance over normal changes
Clinical reassurance matters. Structured wound assessments reduce unnecessary ER visits and panic-driven phone calls.
6. Why Nursing Oversight Changes Outcomes
The gap after discharge is real.
Many complications occur within the first 72 hours at home:
• Missed early infection signs
• Poor drain management
• Incorrect dressing technique
• Inadequate protein intake affecting healing
Nursing oversight ensures:
• Proper wound visualization
• Drain output tracking
• Edema management
• Pain control optimization
• Early surgeon communication when indicated
Surgical success is not only technical. It is postoperative management.
Final Word
If you are recovering from surgery and unsure whether what you’re seeing is normal, do not guess.
Early assessment prevents escalation.
Because the truth about wounds, drains, and dressings is simple
They demand respect.
_edited_.png)



Comments